Fitnesswork.com.au features Karl Lockett
Dealing with Heel Pain
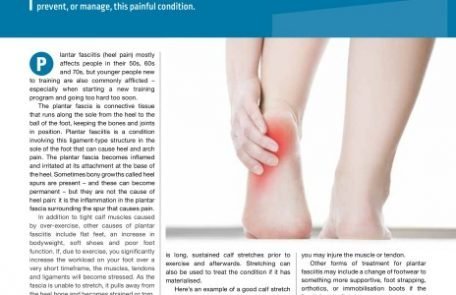
Plantar fasciitis – or heel pain – is not unusual in those new to exercise. Here’s how to prevent, or manage, this painful condition. Plantar fasciitis (heel pain) mostly affects people in their 50s, 60s and 70s, but younger people new to training are also commonly afflicted – especially when starting a new training program and going too hard too soon. The plantar fascia is connective tissue that runs along the sole from the heel to the ball of the foot, keeping the bones and joints in position. Plantar fasciitis is a condition involving this ligament-type structure in the sole of the foot that can cause heel and arch pain. The plantar fascia becomes inflamed and irritated at its attachment at the base of the heel. Sometimes bony growths called heel spurs are present – and these can become permanent – but they are not the cause of heel pain: it is the inflammation in the plantar fascia surrounding the spur that causes pain. In addition to tight calf muscles caused by over-exercise, other causes of plantar fasciitis include flat feet, an increase in bodyweight, soft shoes and poor foot function. If, due to exercise, you significantly increase the workload on your foot over a very short timeframe, the muscles, tendons and ligaments will become stressed. As the fascia is unable to stretch, it pulls away from the heel bone and becomes strained or torn. Plantar fasciitis can also be brought on by long periods of standing or walking, particularly if wearing flat shoes that don’t provide much support. This causes calves to work harder and become tight. The pain associated with plantar fasciitis is often described as feeling like a bruise underneath the heel – like having a stone in your shoe. It is noticed when the foot hits the floor first thing in the morning, and can be so severe that it causes hobbling for a while after getting out of bed.
Prevention and treatment
The best form of prevention for this condition is long, sustained calf stretches prior to exercise and afterwards. Stretching can also be used to treat the condition if it has materialised. Here’s an example of a good calf stretch to be performed for 30 seconds per stretch, three times per leg, and three times per day.
Step 1: One foot back, one foot forward (positioned like a long stride)
Step 2: Both feet point directly ahead
Step 3: Back heel stays on ground – do not lift!
Step 4: Back knee straight
Step 5: Make an arch: roll the back foot to the outside edge slightly to stop foot collapsing, but keep hips centred
Step 6: Don’t bounce, just hold
Stretches are best performed when the muscles are warm and limber. Start gently each time, and don’t over-do each stretch or you may injure the muscle or tendon. Other forms of treatment for plantar fasciitis may include a change of footwear to something more supportive, foot strapping, orthotics, or immobilisation boots if the fascia is actually torn. If your heel pain is due to flat feet or an increase in bodyweight, rather than over-exercise, then you should consult a podiatrist, who can assess whether orthotics are needed to correct the arch and pronation in flat feet, or advise on shoes that can better support extra weight. Karl Lockett is a sports podiatrist and leading specialist in managing heel pain. Offering treatments beyond standard orthotics, including shock wave therapy and dry needling, he is a member of Sports Medicine Australia and the Australian Academy of Podiatric Sports Medicine. www.sydneyheelpain.com.au
Written by Karl Lockett